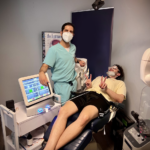
Dr. Silani with a patient administering Lipiflow Thermal Pulsation treatment. Dr. Silani says his practice has gone “all-in” in investing in technologies to provide dry eye care.
By Kambiz Silani, OD
August 3, 2022
I come from a family with a 60-year history deeply rooted in the eyecare and eyewear field. Growing up around eyecare specialists, I decided that medical optometry would be the best fit for me. As someone who has personally overcome multiple medical conditions, embracing a medically oriented optometric practice was an important decision when opening an office.
My goal was to ensure patients receive the highest level of care with a compassionate team while checking both their vision and eye health. So, I set off to learn about, and would slowly acquire, some of the latest technologies available in our profession, from primary eyecare to dry eye.
In fact, over the last nine years, treating dry eye has become a leading priority. To properly diagnose and treat dry eye, I quickly realized the significance of being all in on technology. Being “all in” meant investing in diagnostic equipment and therapeutic devices to strengthen the doctor-patient relationship, as well as creating a treatment protocol that is constantly evolving and consistently applied. Here is how we do it.
Invest in Technology to Provide Advanced Care
Some of our current diagnostic equipment to manage ophthalmic diseases includes the Cirrus HD-OCT (Zeiss), VF2000 visual field analyzer headset (Micro Medical Devices), VX 120 anterior segment analyzer (Visionix), Keratograph 5M (Oculus USA), Firefly Slit Lamp (Eyefficient), Nidek retinal camera and Optos wide-angle retinal imaging. Some of our current therapeutic devices include TearScience LipiFlow (Johnson & Johnson Vision), OptiLight (Lumenis), TearCare (Sight Sciences), iLux (Alcon), BlephEx and ZEST (Zocular eyelid treatment system).
Our dry eye center is now fully equipped with modern evidence-based devices, but it wasn’t always this way. Initially, we relied on very minimal tools for evaluating and managing dry eye. However, we quickly found that more advanced diagnostics and office-based treatment options were needed to address the multi-factorial nature of dry eye effectively.
Screen All Patients for Dry Eye
Our current “all-in” approach to ocular surface disease includes catering to a wide-ranging patient population, from students to celebrities. Some may have only subtle signs of dry eye that become apparent during an annual exam, while others have visited multiple specialists and are truly suffering from symptoms that might include dryness, itch, redness, epiphora, sties, contact lens discomfort and fluctuating vision.
When patients present for their initial consultation, it is comprehensive and extensive. History taking includes current and past information about pets, allergies, home and work environments, cosmetic products, contact lens wear, time spent on screens, medications, systemic and skin condition, etc. Nearly every patient undergoes vital dye staining, manual expression of the meibomian glands, TearLab osmolarity testing, InflammaDry MMP-9 testing (Quidel), meibography and advanced corneal imaging with the Oculus Keratograph 5M.
We also use the Firefly slit lamp, which gives us the ability to show patients and their families what we see at the slit lamp, either in real time, or in videos they can watch later (see video). These images, combined with meibography, are a wonderful patient education tool and help us to build trust in our recommended treatment protocols. Treatments are offered on the same day as the consultation, if patients are ready to proceed.
Implement a Treatment Protocol
We prefer to address the root causes of ocular surface disease with office-based procedures rather than lifelong topical medications. In fact, if patients are on chronic drops for dry eye, one of our goals is to get them off the drops. Treatment decisions fall into three categories for us:
1. First, we carefully examine the lid margin. If the patient has anterior blepharitis, biofilm, evidence of Demodex mites and/or abnormal staining of lissamine green around the meibomian gland (MG) orifices, we recommend microblepharoexfoliation with BlephEx or the more manual ZEST procedure. This is a great way to get rid of external debris that can block the flow of healthy meibum through the MG orifices.
2. If the patient has ocular rosacea or significant inflammation, we recommend a series of IPL treatments, typically with the FDA-approved OptiLight. Following each IPL session, we perform manual expression under a topical anesthetic. This is primarily diagnostic, as it allows me to evaluate the expressed meibum and determine whether a heat-based treatment is necessary. This process is captured for the patient at the Firefly slit lamp.
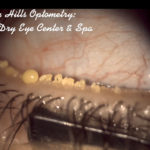
Fig. 1: In-office diagnostic expression shows that this patient has obstructive MGD that should be treated with a heat-based treatment such as TearScience LipiFlow.
3. If the meibum consistency is anything other than clear, liquid oil, the patient has obstructive MGD that should also be treated (Fig 1). We explain to patients that we need to do a heat-based treatment to extract the “gunk” that is contributing to their symptoms. IPL alone is limited in heating the meibomian glands to a therapeutic level and is not sufficient to address truly obstructed, inspissated glands. For that, we need more advanced thermal treatments.
In most cases, we use TearScience LipiFlow (Johnson & Johnson Vision), because it provides simultaneous external pressure and internal heat, has the longest track record and is, by far, the most extensively studied. However, we also offer exceptional alternatives such as iLux (Alcon) and TearCare (Sight Sciences), especially for patients who are not candidates for TearScience LipiFlow, such as those with very small eyelid fissures, claustrophobia, keratoconus or an active chalazion or hordeolum.
As these three treatment categories are synergistic, some patients may benefit from having multiple treatments at their initial visit, but we can also proceed in a step-wise fashion when there are time or financial constraints. About 80-90 percent of patients do well with a combination of the treatments above, plus a home-care regimen (see sidebar).
Learn More
Click HERE to download Dr. Silani’s “Expectations for Treatment for Moderate-to-Advanced Multifactorial Dry Eye.”
We share with patients that if they can’t comply with the home routine, we may need to be more aggressive with office-based treatments—just like they might need more frequent dental appointments if they aren’t flossing and brushing regularly at home or if they are more prone to plaque/tartar buildup. In some cases, we may also consider punctal occlusion (almost never as a first-line option), an amniotic membrane bandage (Prokera, BioTissue), or a short 2- to 4-week course of loteprednol etabonate 0.25% (Eysuvis, Kala Pharmaceuticals) for symptom flareups.
You will often hear that patients may require a TearScience LipiFlow treatment once a year or TearCare every six months, but it is important to remember that these are averages. Some patients may benefit for years from a single treatment, while others need more frequent treatments. We also explain to patients that, in rare occasions, they may actually feel worse before they feel better, and that they have to trust in the process.
Other Articles to Explore
You Can Start Small & Build to “All In”
Not every practice will have the bandwidth to go all in, as we have. But I encourage colleagues to at least evaluate both structure and function. At the most basic level, this can be done with lissamine green, a slit lamp and manual expression. Meibography is perhaps the most useful first advanced diagnostic tool to add, and then one can expand to treatment devices. While the financial cost of entry for devices like TearScience LipiFlow or OptiLight is relatively high, the return on investment for the practice is also high. More importantly, the benefit to the patients is tremendous.
 Kambiz Silani, OD, is Chief Clinical Director of Beverly Hills Optometry, a specialty practice with an advanced dry eye center in Beverly Hills, Calif. He is a consultant for Johnson & Johnson Vision, Alcon, Sight Sciences, Lumenis and NuLids. To contact him: info@bheyeguy.com.
Kambiz Silani, OD, is Chief Clinical Director of Beverly Hills Optometry, a specialty practice with an advanced dry eye center in Beverly Hills, Calif. He is a consultant for Johnson & Johnson Vision, Alcon, Sight Sciences, Lumenis and NuLids. To contact him: info@bheyeguy.com.





















