By Richard Edlow, OD

April 14, 2021
Mississippi has become the sixth state in the country to permit qualified ODs to perform laser eye surgery, joining Arkansas, Alaska, Oklahoma, Louisiana and Kentucky.
In addition, Florida’s House Professions and Public Health Subcommittee recently advanced a bill that would allow optometrists to perform certain eye surgeries and prescribe an expanded list of medications. Expansions in scope of care in these states represent a significant step forward in providing patients expanded access to primary care health services. They also elevate ODs’ scope closer to the profession’s current level of education and training. Here are points to consider as we enjoy greater expansion of scope of practice while continuing to share the marketplace with other eyecare providers.
Fulfilling a Need for Many More Eyecare Providers
What do these newly heightened privileges say about say about future directions for optometry and market-driven challenges in store for the entire eyecare delivery system? The solution is relatively simple and obvious. The problem is as well.
As the U.S. population ages, the demand for office based age-related eyecare services will increase by more than 30 percent from 2020 to 2030 and with an additional 33 percent increased demand for cataract surgery. Earlier this month (March 2020) Mississippi became part of the solution. Let me explain.
Every year in the U.S., ophthalmology residency programs produce 490 brand new ophthalmologists. Every year somewhere in the ballpark of 425 ophthalmologists retire or exit the profession. That net increase of 65 new surgeons each year, for the entire country, will result in just a paltry 3 percent increase in the supply over the entire decade (2020-2030). It is virtually impossible for this essentially flat supply of surgeons to meet the demands of the 30 percent and 33 percent increase in services and surgery. This doesn’t include the increase in diagnostic testing and interpretation or the continued expansion of intra-vitreal injections.
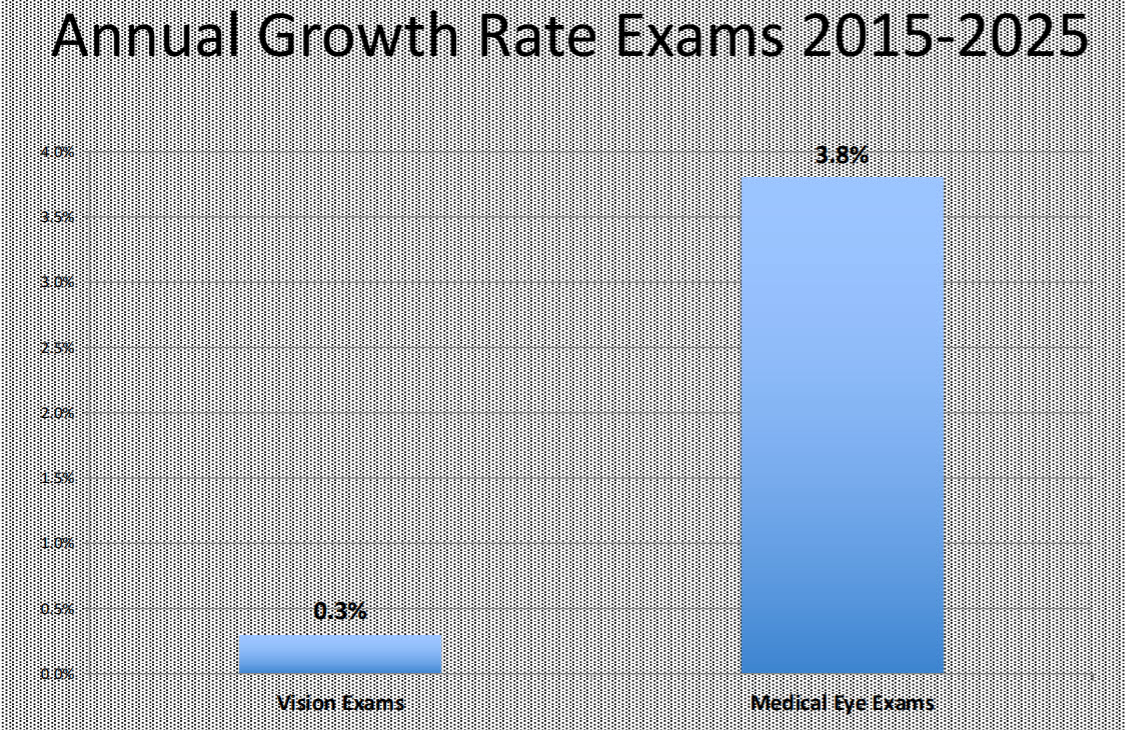
Are ODs Up to the Challenge?
Based on Centers for Medicare & Medicaid Services (CMS) Utilization & Payment data, as well as U.S. Census Bureau projections, I estimate that eyecare providers need to deliver an additional 16 million medical eye exams and 10 million diagnostic tests EACH and EVERY YEAR for the next 10 years.
How Scope of Care is Expanding
Cataract surgery volume in the U.S. was approximately 4.2 million procedures in 2020 (adjustments for COVID-19 will most likely result in a lower number once all the data is in). It is expected to reach 5.6 million procedures by 2030. The average procedure volume for general ophthalmologists and anterior segment specialists is in the ballpark of 400 cases per year. The increase of 1.4 million procedures by 2030 would require an additional 3,500 surgeons. However, the net increase of 65 surgeons per year will only supply 650 surgeons by 2030 and that number is reduced by those sub-specializing in the various ophthalmology specialties (e.g., neuro, cornea, oculo-plastics, peds, retina, etc.)
Proper access to care will require that optometry fill the void that ophthalmology will create as surgeons are driven increasingly into the operating room for invasive intraocular procedures from cataract surgery to retinal repairs. As novel as this may sound, ophthalmology ought to embrace scope of practice expansion like Mississippi’s for the sake of overall public health and their very own professional well-being and efficiency. Mississippi now joins 20 other states with expanded scope that very clearly are part of the solution to providing proper access to eyecare.
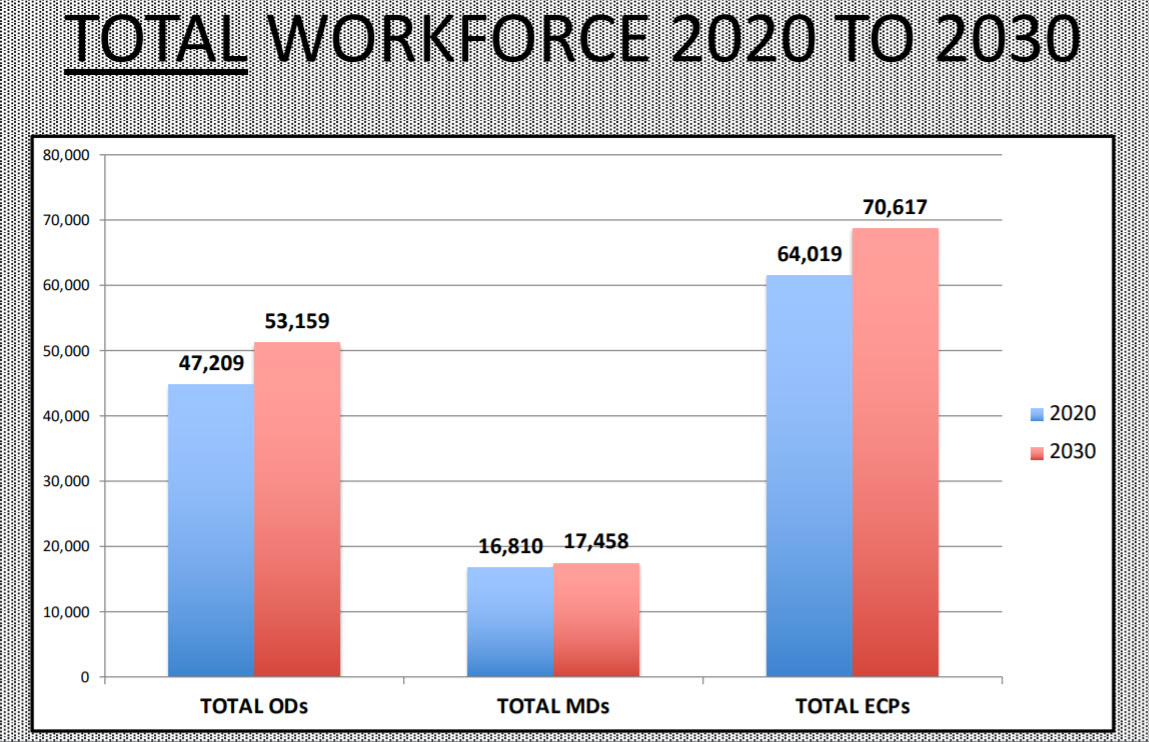
Time to Collaborate to Ensure the Availability of Care
Marketplace dynamics will surely force a continuation of this trend. Perhaps it is time for a national summit of leaders in both professions to come together, and study the facts and data available, to develop a collaborative care framework that addresses not optometry as one professional silo and ophthalmology as another, but, instead, a delivery system for all eyecare as a single industry with a team of providers acting in concert. The joint collaborative care team could develop clinical guidelines that address increasing patient demand for medical eyecare services, optometry’s full extent of clinical training in conjunction with the growing relative supply shortage of ophthalmologists.
Other Articles to Explore
From a public health perspective, we cannot afford to delay this collaborative care approach.
 Richard Edlow, OD, known as the Eyeconomist, recently retired from clinical care. To contact him: redlow@aol.com
Richard Edlow, OD, known as the Eyeconomist, recently retired from clinical care. To contact him: redlow@aol.com



























