
The Optos retinal camera in Dr. Krivacic’s office. Dr. Krivacic says the technology both elevates patient care and builds revenues.
By Ken Krivacic, OD, MBA
June 17, 2020
Your patients benefit from advanced diagnostic technology, and so can your practice.
Here is the technology investment that is enhancing patient care and generating many times the amount of money we invested to acquire it.
What Is It?
The Optos Daytona is the best instrumentation investment we have made in our practice, which has 2.5 full-time ODs working in a single location. We invested in it because we thought it would be a great way to photo-document the retinas of our patients, and that it would be a great practice builder if presented properly.
Along with being a practice builder, this instrument improves the standard of care a patient receives from your office versus an office that does not photo-document. It shows that you value the health of the patient’s eyes and have made that a part of your routine
How Much Did It Cost?
We purchased our camera. The cost at the time was just under $84,000 and we financed it over five years. The monthly payments were around $1,531 per month. That sounds daunting, but if you can promote the scans and do enough volume, the return on investment is impressive.
The instrument takes up about a 4 sq. ft. of space and can be pushed up against a wall. We have our instrument in one of our pre-testing rooms.
 What Has the ROI Been Like?
What Has the ROI Been Like?
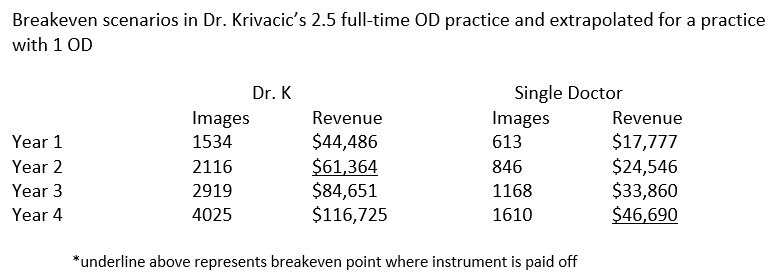
The instrument paid for itself almost immediately. With our volume of patients, we perform an average of 325 retinal images per month.
The majority of those are screening images for which the patient pays an out-of-pocket fee of $29. This results in monthly revenue of just short of $10,000 per month. We broke even with the instrument in 20 months. Of course, a key advantage in our practice is we have three doctors who can generate photos.
How would this equate to a single doctor in a single location? If we extrapolate the numbers, the breakeven for a single doctor is around 42 months. This is still a good investment as the instrument will probably have a lifespan of at least seven years and anything after the breakeven point is pure profit.
How Do You Get Reimbursed?
About 90 percent of our retinal photos are screenings, so there is no third-party billing. The other 10 percent are considered medical photos, which require an accompanying report and are billed medical. We use procedure code 92250.
Present the Retinal Photo Option to All Patients
Our tech staff presents the photo option to all patients, and they take the photo. The photo is then linked to our exam rooms where the doctors review the photos with patients and explain the advantage of having a photo to document the internal history of the patient’s retina.
Other Articles to Explore
We came up with our own script on how we would like it presented to our patients, personalized to our practice. This is important and can be the difference in how well you utilize the instrument. The doctors and staff need to be on board as to why the instrument is beneficial to patient care. If it is only there to generate income, it will be a much harder sell to doctors, staff and patients. All three groups need to know there is a good reason to have a photograph in the patient’s chart.
Since most of our images are screenings, we promote it as a great way to document what we see in the patient’s eye. The patient is told the image will be saved and then when they return next year we will be able to do a year-to-year comparison.
As a doctor, I tell the patient it helps me because I can look inside the eye and write down what I see, but if I have a photo it is much easier for me to compare what the eye looks like from year to year. This helps me detect any early changes that may occur.
Doctor Needs to Be a Patient Educator
Patients also need to be shown the images and have them explained. Here the doctor needs to behave like an educator. In most standard optometric practices we are working with healthy patients. In this scenario, the doctor needs to become a teacher to show the benefits of the photos.
In our practice, we do this by bringing up the images on our computer screen in the exam room and having the doctor review basic ocular anatomy. We have an eye model on our exam room desks to help explain how the image is obtained and to give the patients a 3-D model of what they are viewing on a flat screen. Some patients can be confused as to what you are showing them, so again, make sure you teach.
We review basic structures like the optic nerve, macula and blood vessels. This is important because, with technology advancing, it is not unreasonable in the not-too-distant future that patients will obtain an online image of their retina. For us as clinicians to remain viable we need to explain those images to the patient. I also believe that moving forward most patients will still prefer the personal touch and a doctor who will explain to them what makes their eyes unique.
 Ken Krivacic, OD, MBA, owns Las Colinas Vision Center in Irving, Texas. To contact him: kkrivacic@aol.com.
Ken Krivacic, OD, MBA, owns Las Colinas Vision Center in Irving, Texas. To contact him: kkrivacic@aol.com.





















