By Mark Wright, OD, FCOVD,
and Carole Burns, OD, FCOVD

Feb. 10, 2021
Every year it is important to go through an exercise with the Medicare Physician Fee Schedule. If you are a Medicare provider, this details what Medicare reimbursement is for each CPT code. From this we can determine what the patient is responsible for today and what Medicare will send to you in a check (if your fees meet or exceed the Medicare reimbursement).
The very last thing you want to do is to increase your accounts receivable by telling patients that you will bill them once a third party tells you what they owe. Do this exercise so, with Medicare patients, you will never be in that situation.
To start this exercise, follow this path:
Overview of the Medicare Physician Fee Schedule Search | CMS
Left click the BEGIN SEARCH button.
Left click AGREE.
Enter the search parameters (for our purposes we will search for 99202-99205 to start).
Here’s what this will look like:
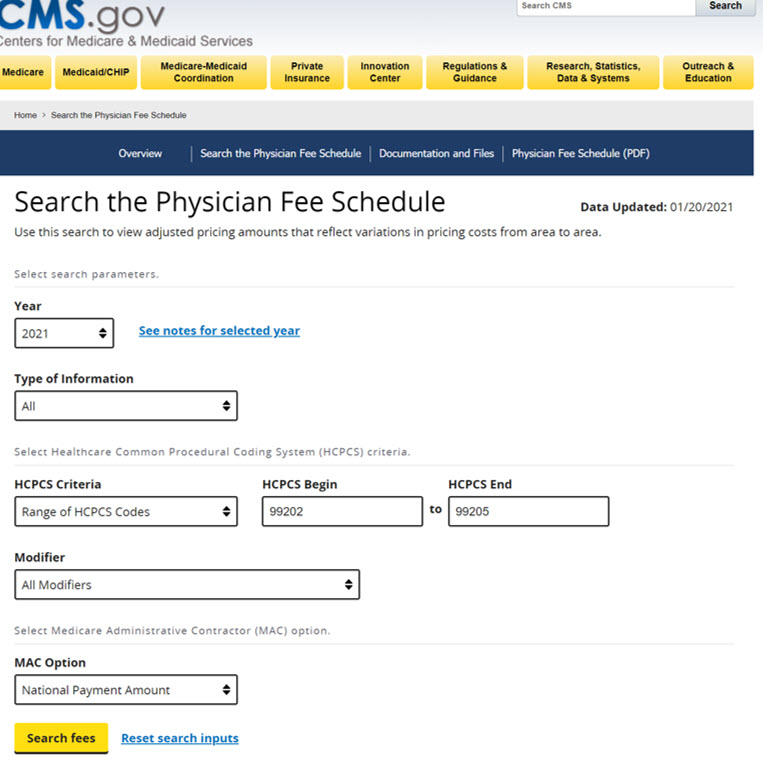
NOTE: For this example, we’ve chosen the following key parameters:
• Under the HCPCS Criteria you can choose between Single, List or Range – we chose Range.
• Under the MAC option “National Payment Amount” (you should choose “Specific Locality” for your practice).
After entering your codes, then left click the SEARCH FEES button and it will return with this:

The Non-Facility Price is the Medicare reimbursement for out-patient care (this is what you deliver in your practice). Put the codes and the reimbursement rates into a spreadsheet. It should look like this:

By adding an 80 percent and a 20 percent category to your spreadsheet, you will have identified the 20 percent co-pay the patient is responsible for as well as the 80 percent that Medicare will pay after the deductible is met.

You can use this process to determine the Medicare fees for any code. Let’s repeat this process with codes 99212-99215 for established patients. It will look like this:


Putting this new information into the spreadsheet you are creating gives this result:

Other Articles to Explore
Medicare reimbursements change every year. Going through this exercise enables you to handle E/M code reimbursements for any Medicare patient entering your office who has met their deductible. Do this every year.