By Ian Ben Gaddie, OD
Sept. 27, 2017
Glaucoma care is a growing need in the U.S, with the The National Eye Institute estimating that by 2030, 4 million Americans will have glaucoma, and by 2050, 6 million will.
I’m seeing a prevalence of glaucoma in my own community of Louisville, Ken., where 60-70 percent of my 10-OD, four-location practice is devoted to glaucoma care. With the especially high incidence of the disease among African-American and Hispanic populations, if your practice is based in a diverse community, an even greater percentage of your patient base could be glaucoma suspects than what I’m seeing in Louisville.
As a sight-threatening condition, it is a service to patients to diagnose and treat the disease, and it also happens to be a practice- and profitability-builder. Treating a chronic eye disease becomes an annuity to the practice, and contributes to growing the medical side of the practice at a time of waning retail opportunities.
Implement Protocol
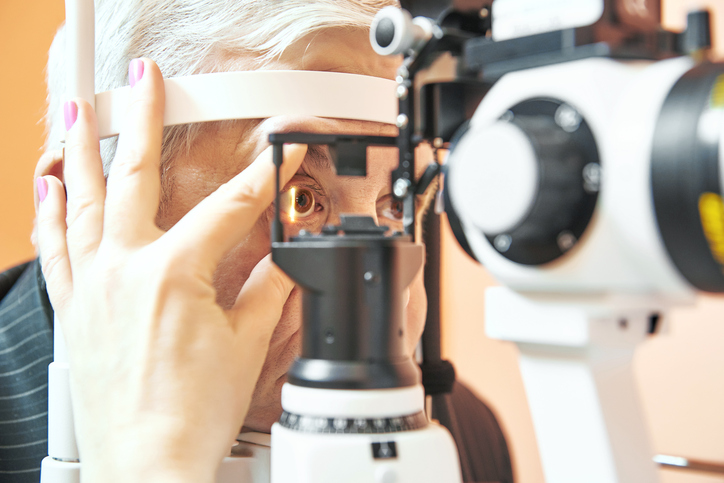
Once diagnosed, my glaucoma patients visit our office three times a year, or every four months. Two of those visits are to monitor intra-ocular pressure, and the third visit is to perform a visual field and OCT to monitor the progression of the disease.
Laws regulating glaucoma care vary by state, but as an OD in Kentucky, the only time I need to send the patient to another doctor is if the patient needs glaucoma-related surgery. Occasionally, I will send the patient to another doctor to get a second opinion on the diagnosis and treatment plan.

Click HERE or the image above to read how Dr. Gaddie saved time, and generated revenue, with wavefront autorefraction technology.
Optimize Doctor Time: Delegate Testing
A full evaluation of a glaucoma patient takes 20-30 minutes to do all the testing, which I delegate to my support staff, and 15 minutes for me to interpret the findings and review with the patient. If the patient is only coming in for a pressure check, rather than the full evaluation, the visit may only take a few minutes of support staff time. If the patient coming in for a pressure check also is having difficulties with the medication I prescribed, than that visit, too, could require additional doctor time.
My associate and I have trained our staff how to guide glaucoma suspects, and patients, through testing. One of the ways we do that is by having them sit in the exam room with us when we educate glaucoma patients about their disease. We also send our pre-testing technicians to continuing education courses on glaucoma care. Once staff are trained, they can then help train other employees.
Schedule to Maximize Efficiency
Some doctors like to have a half-day, or full day, once a week, to devote to glaucoma patients. In my practice, I’ve found that it’s most efficient to integrate care of these patients into the rest of our schedule. With visits just for pressure checks only requiring a few minutes, we are able to easily work those visits in between comprehensive exam slots. Having support staff that can assist with those pressure checks helps keep glaucoma care profitable by avoiding unnecessary use of doctor time.
When you first add glaucoma care to your practice, be conservative in the amount of time left open in your schedule for those visits, and as you ramp up, you can always add additional appointment slots.
Share Advanced Instrumentation with Other Practices
Some of the technology available to treat glaucoma patients is costly. For instance, the selective laser trabeculoplasty instrument is around $80,000 to purchase, and reimburses at around $300 per procedure. My practice shares use of that instrument with other optometrists and ophthalmologists at a local surgery center. In Kentucky, an OD is permitted use of this technology to treat patients.
We schedule all of our cases requiring treatment utilizing the surgery center on one or two days a month to simplify our arrangement with the other practices we share the equipment with.
Gain Confidence as a Glaucoma Care Provider
I find in speaking with other optometrists that, despite the medical eyecare training they received in optometry school, many lack the confidence to diagnose and manage the disease.
To gain that confidence, I recommend spending the day shadowing a doctor with many glaucoma suspects and patients. Ask to sit in the exam room as the diagnoses are made, and when the patient education occurs. If you don’t know an OD with a glaucoma specialty in your area, you can also ask to shadow an ophthalmologist focusing on glaucoma care.
There is a longstanding trend of ODs referring glaucoma patients to general ophthalmologists who don’t specialize in managing the disease. Outside surgical needs, that shouldn’t be happening. This is a chronic disease that optometrists should own.
Market Glaucoma Care
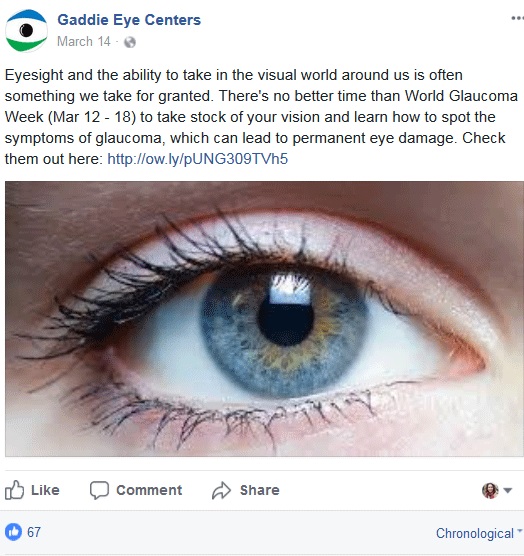
One of the ways we let our community know about our glaucoma care is through social media posts on our practice Facebook page with information about the disease. Here is an example of a post from earlier this year, to mark World Glaucoma Week:
And here is an example of the kind of educational post we run throughout the year on the disease:

 Ian Ben Gaddie, OD, is the owner of Gaddie Eye Centers in the Louisville, Ken., area. To contact him: ibgaddie@me.com
Ian Ben Gaddie, OD, is the owner of Gaddie Eye Centers in the Louisville, Ken., area. To contact him: ibgaddie@me.com