By Mark Wright, OD, FCOVD,
and Carole Burns, OD, FCOVD

August 15, 2018
ODs are incorporating video, and use of mobile technology, in how they educate, and work with, patients, according to Jobson Optical Research’s 2017 ECP Digital Solutions Study.
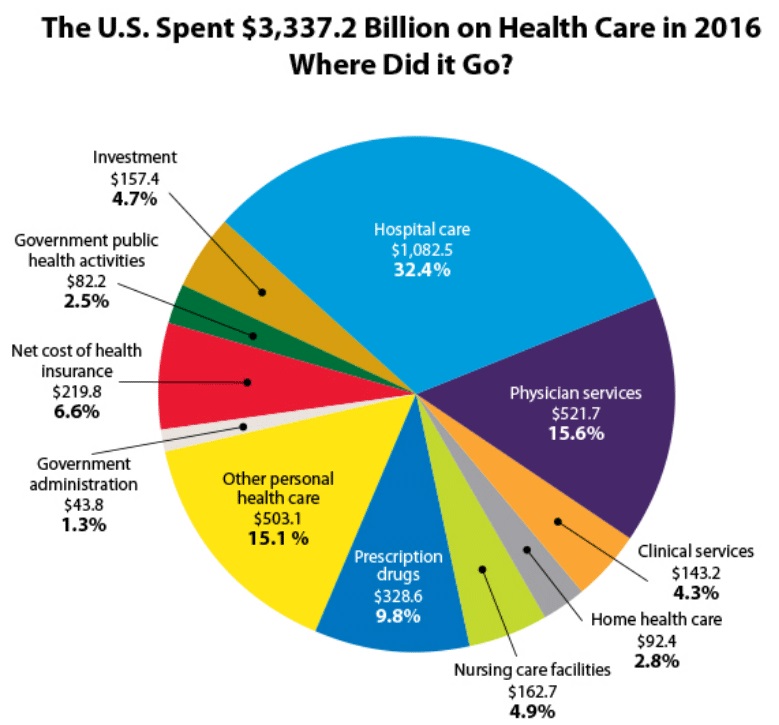
A lot of money is spent on healthcare each year. Two reasonable questions are: where did the money go and can we do better? Where did the money go?
The illustration below gives us the answer to where the money went.
Can we do better?
In the mid-1990’s, Bartlett did a meta-analysis of studies up to that point and showed that for every $1 spent on patient education, between $3 and $4 were saved. We’ve known for over 20 years that patient education improves care and saves money.
Patient education is one of the answers to how we can do better. Current patient education is centered around patient empowerment. Patient empowerment is more than just explaining the diagnosis and treatment plan to the patient. Patient empowerment is about helping patients to take control and manage their own health – to care about and invest in improving their quality of life. The value of this approach is that it may permit patients to modify the course of their disease, have fewer complications, and ultimately, to have lower health-care costs.
Two of the barriers to patient education have been that we overwhelm patients with information and the limited time patients have during an office visit for questions and answers. Both of these barriers can be effectively addressed with the use of video and mobile digital technology.
We have moved from a relatively quick discussion with the patient and handing them a brochure to some amazing technology advances to help patients understand and take control of their own health. Here are a few examples of these changes.
“Louise” is a virtual nurse created in 2008 at Northeastern University to provide an interactive discussion with patients about home care. Here are the key findings from that experience:
• It freed up physician time.
• It saved the hospital $145 per patient.
• 74 percent of interviewed hospital patients preferred to get information from “Louise” rather than the physician.
In 2012, an innovative first-person simulation using 3D headsets for patients showed the high impact of mild hypoglycemia on a patient. The simulation made the viewer “feel” the symptoms of hypoglycemia throughout a typical day for a person with type 2 diabetes. This gave patients greater understanding of low blood sugar symptoms and resulted in patients taking action sooner to address blood sugar issues.
There are many eye specific apps available for both iPhone and android devices. Click HERE for a listing of eye related apps such as: Vision Aids and Tests; Visual Impairment and Blindness; Pricing and Reminder Apps; Hospital Locators; Optical Illusions and Fun; Color Vision Deficiency; Cosmetic and Try-on; Quit Smoking; and Vision Development. Some are free and some require a fee.
The other advances in patient education that are here now, which you should consider, are e-learning and remote monitoring. Both of these will change how we empower patients as we move forward in time.
Today, videos and digital illustrations that can be displayed on everything from large screens in the office to smartphones at home are commonplace. These can be accessed in your reception area, on your web site, or on digital devices anywhere. You can show them to patients in the office, or even “push” them to patients through digital communications for viewing (or reviewing) at their leisure.
All of these tools for helping patients understand and take control of their own health will increase in number and quality over time.
How many of these advances in patient education are you routinely utilizing for patient empowerment? Take this week to review what you are doing in this area, and see if there are improvements that can be made.
References
i. Bartlett E, Patient Education and Counseling 26, 1–3, 1995, Pages 87–91
ii. Jack, B.W et al. A reengineered hospital discharge program to decrease rehospitalization: A randomized trial. Ann Intern Med, 2009 150(3), 178-187.
iii. http://www.pmlive.com/pmhub/medical_communications/fti_consulting/white_papers_and_resources/how_technology_is_shaping_patient_education